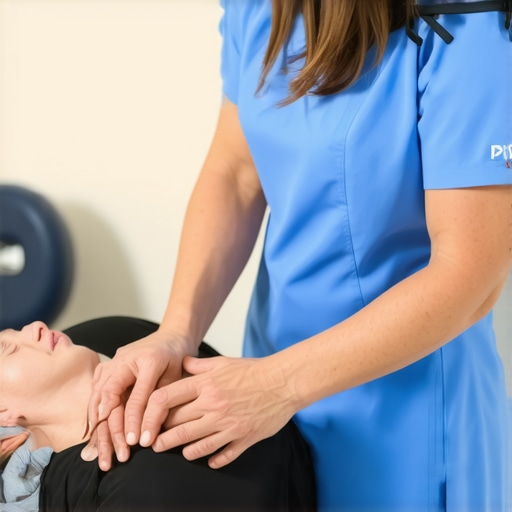
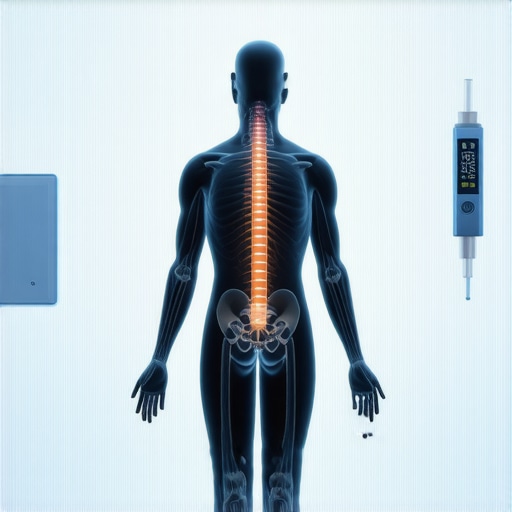
Imagine lacing up your sneakers, eager for that refreshing morning ritual. You step outside, muscles tense with anticipation, only to feel that all-too-familiar jolt in your lower back, shooting down your leg. That sting, that numbness—it’s become a part of your routine, almost like an unwelcome companion. I remember the first time I experienced it: a seemingly innocent walk turning into a painful ordeal. It was a lightbulb moment for me, realizing that some of my morning habits might be doing more harm than good.
The Real Reason Your Morning Walk Might Be Making Your Sciatica Worse
Many of us believe that staying active helps, but for those dealing with sciatic nerve issues, the wrong kind of activity can actually aggravate symptoms. I learned this the hard way, making a classic mistake early on—pushing through pain without understanding its root cause. That misstep led me to research and discover that specific movements and postural habits during morning walks could intensify nerve irritation rather than ease it. It’s a common pitfall, and unfortunately, one that keeps many stuck in a cycle of discomfort.
Did you know that poor posture during daily activities like walking can contribute significantly to ongoing sciatica pain? According to a research article, sustained bad posture places additional pressure on the spine and nerve roots, worsening sciatic symptoms. This means that your morning routine might need a closer look—are you walking with proper alignment, or could your habits be contributing to the problem?
Think It’s Just About Moving More? Think Again.
Many swear by morning walks as a cure-all, but if you’re not careful, they could be shifting from health boost to pain trigger. I’ve found that understanding the nuances of proper movement and posture is key. Small adjustments in how I walk and stretch have made an enormous difference. The goal isn’t to stop exercising but to do it smarter—more in tune with your body’s limits and needs.
So, before you dismiss your morning walk as a harmless routine, ask yourself: Are my movements helping or hurting my recovery? If you’ve faced this dilemma or want to ensure your walk is part of a healing process, keep reading. We’ll explore practical strategies and expert tips to transform your morning routine into a safe, effective step toward relief—without risking further nerve irritation. And if you’re eager to dive deeper into lifestyle changes that support your journey, I recommend checking out some of the targeted approaches outlined in our comprehensive guides on boosting mobility and reducing pain.
Start With Posture Checks
Before stepping out, assess your posture. Stand tall, shoulders relaxed, ears aligned with your shoulders. Imagine a string pulling your head upward—this keeps the spine in proper alignment. I once overlooked this, and during a morning walk, I felt a sudden jolt in my lower back, which prompted me to correct my posture. The next day, my discomfort reduced significantly because I began consciously maintaining good posture during walks.
Engage Your Core During Walks
Think of your core muscles as a foundation or a sturdy scaffold holding up a building. Activating these muscles stabilizes your lower back and reduces nerve pressure. During an early attempt, I focused solely on my legs, but after learning to engage my abs gently (by imagining pulling my belly toward my spine), I noticed less sciatic pain. To do this, tighten your abdominal muscles slightly, hold briefly, then relax. This prevents excess strain on your lower back with each step.
Control Your Gait and Footfall
Examine how you walk. Aim for a heel-to-toe rolling motion. Imagine your foot as a piston—land softly on your heel, roll smoothly over the arch, push off with your toes. I made it a habit to walk at a moderate pace, avoiding quick, pounding strides which often worsened my sciatic symptoms. Faster steps or heavy landings increase impact and nerve irritation. Practice consciously lightening your footsteps for a more controlled gait, reducing nerve compression risks.
Introduce Gentle Stretches at the Start and End
Stretching enhances flexibility and reduces muscle tightness contributing to sciatic pain. For instance, I added gentle hamstring and hip flexor stretches—key areas affecting sciatic nerve pressure. Bend over slowly, reaching for your toes, but avoid bouncing. Also, perform a seated piriformis stretch by crossing one leg over the opposite knee and gently leaning forward. These stretches can alleviate nerve compression, but remember, over-stretching can aggravate pain—proceed gradually.
Adjust Walking Surface and Pace
Walking on softer surfaces like grass or gravel absorbs shock better than concrete. I rotated my routine to include parks instead of sidewalks, which made a noticeable difference. Also, keep a steady, moderate pace rather than rushing or walking too slowly. Sudden speed changes can strain muscles or cause awkward gait patterns that worsen sciatic symptoms. Experiment to find a rhythm that feels comfortable and sustainable, not exhausting.
Implement Proper Breathing Techniques
Deep, diaphragmatic breathing enhances oxygen flow and reduces stress—both factors affecting pain perception. During your walk, focus on slow inhales through your nose, expanding your belly, then controlled exhales. I remember a morning walk where paying attention to my breath not only calmed my nervous system but also helped me maintain better posture. Incorporate this habit to support overall nerve health.
Limit Walk Duration and Intensity
Overdoing it can rebuild inflammation and tighten muscles. Start with short, 10-15 minute walks, then gradually increase as your body adapts. I once pushed myself for 45 minutes too soon, which resulted in increased numbness. Listening to your body’s signals is crucial—discomfort isn’t a sign to push harder but to slow down. Use a timer or a fitness tracker to keep your walk duration manageable, and avoid incline terrains initially to reduce impact.
Maintain Consistency and Review Progress
The key to transformation is regularity. Establish a routine—walk 3-4 times a week—and keep a journal to note changes in pain levels, mobility, and posture. I found that tracking my experiences helped identify which techniques provided relief. Over time, small adjustments, like refining my gait or adding new stretches, compounded into significant improvements. Keep an open mind, and consult resources like simple exercises that make a difference to guide your progress.Many people believe that sciatica, neck pain, and back issues are solely a matter of muscle strain or injury, but the truth is often more nuanced. A common myth is that pain always indicates damage that needs to be completely restayed or immobilized. In reality, controlled movement and targeted exercises often promote recovery, as emphasized by experts in physiotherapy. For example, prolonged bed rest can actually hinder healing, leading to stiff joints and weaker muscles, which may exacerbate pain over time. Another prevalent misconception is that stretching is universally beneficial; however, overstretching or improper technique can worsen nerve irritation, especially if done without guidance. As discussed in research published in the Journal of Orthopaedic & Sports Physical Therapy, individualized assessments are crucial to determine appropriate interventions. It’s vital to recognize that advanced mobility strategies involve understanding the body’s feedback mechanisms—listening to discomfort signals to prevent further injury. This prevents falling into the trap of overdoing passive stretches or simplistically assuming that more movement is always better. Instead, focusing on gentle, proprioception-enhancing exercises can improve outcomes significantly. Moreover, many assume that pain is always linked to structural damage, but in chronic cases, pain may be driven by neural sensitivity or stress-related tension, as detailed in studies on central sensitization. This explains why addressing stress, emotional health, and posture can dramatically influence recovery. Have you ever fallen into this trap? Let me know in the comments. To explore effective ways to manage and prevent these issues, visit our cornerstone guide on improving mobility and reducing pain for lasting relief.
Maintaining your progress against sciatic pain, neck discomfort, or mobility issues requires reliable tools and consistent routines. Over the years, I’ve found that integrating specific equipment and techniques can make the difference between short-term relief and lasting health. One of my go-to tools is the foam roller. I prefer the foam roller because it helps release muscle tightness, particularly in the hips and lower back, which are often culprits in nerve irritation. Regular self-myofascial release using a quality foam roller has significantly reduced flare-ups and improved my mobility over time. Another essential item is a lumbar support cushion. When I sit for extended periods, whether working or driving, this cushion helps maintain proper spinal alignment and prevents additional pressure on the sciatic nerve.
Invest in Proper Software and Apps
For tracking your progress and staying motivated, I recommend using specific apps that focus on posture, mobility, and stretching routines. Apps like posture correction or guided mobility programs help remind you to perform gentle exercises regularly, which is crucial for long-term results. These digital tools can also identify patterns in your pain levels, guiding adjustments in your routine. As technology evolves, we can anticipate AI-powered apps offering personalized movement plans tailored to your unique needs, making sustained management even more accessible.
Why Consistent Practice Is Key
Ultimately, the real secret to lasting relief lies in consistency. I make it a point to dedicate a few minutes daily to mobility exercises, stretching, and using my tools correctly. This habit compounds over weeks and months, reinforcing healthy movement patterns and reducing the chances of setbacks. If you’re wondering, lifestyle adjustments like ergonomic improvements and regular movement become much more manageable when paired with the right tools.
How do I keep long-term relief sticking around?
To sustain progress, review your routine periodically, refine your exercises, and invest in quality equipment. Don’t forget to revisit your posture habits and adapt your workspace to prevent recurring strain. Combine these with targeted practices like gentle strengthening exercises and deep breathing techniques—practices shown to influence neural sensitivity positively. For instance, mobility-focused strategies improve both pain management and overall function. Consider trying a simple technique like using a foam roller on those tense hip muscles before it leads to nerve pressure. The key? Make it a non-negotiable part of your routine. As experts suggest, consistent maintenance not only preserves progress but also prepares your body for future challenges. Stay proactive: schedule weekly check-ins, revisit your ergonomic setup, and continue practicing the exercises that work best for you. Remember, the goal isn’t just relief but resilience. By combining this approach with ongoing education and community support, you can keep your body working efficiently for the long haul. Prioritize your health, and you’ll find that even chronic issues become more manageable over time. For more advanced strategies and personalized guidance, explore comprehensive resources and consider consulting a qualified physical therapist. Now, take one step: pick your favorite mobility tool and use it today to reinforce your progress—small consistency wins lead to lasting freedom from pain.
The Hardest Lesson I Learned About Sciatica, Neck Pain, Mobility, and Back Pain
One of my most eye-opening realizations was that pushing through pain often worsens the condition, rather than helps it heal. I used to think that extra effort meant more progress, but I discovered that listening to my body’s signals and respecting its limits accelerated my recovery. Embracing gentle movements and patience proved more effective than forced exertion, especially when managing sciatic nerve irritation.
How Small Adjustments Transformed My Mobility Journey
Adjusting my posture during walks and incorporating targeted stretches made a significant difference. Simple tweaks—like engaging my core or consciously lightening my steps—created noticeable relief over time. This taught me that tiny, consistent changes in daily habits can powerfully impact long-term health, turning a routine walk into a therapeutic ritual rather than a pain trigger.
My Eye-Opening Mistake About Over-Stretching
I once believed stretching was always beneficial, but I learned that over-stretching or improper technique could inflame nerves. Guided by expert advice, I shifted to gentle, proprioception-focused exercises. This prevented setbacks and kept me motivated, underscoring the importance of personalized, cautious approaches rather than generic routines.
The Unexpected Role of Stress and Neural Sensitivity
Discovering that neural sensitivity and stress influence persistent pain shifted my perspective. Addressing emotional well-being through deep breathing and mindfulness complemented physical routines, leading to a more holistic recovery. Recognizing the mind-body connection helped me stay resilient during setbacks and reinforced that healing isn’t just physical—it’s emotional too.
What Resources Keep My Journey on Track
My trusted tools include a high-quality foam roller for muscle release, ergonomic cushions to maintain proper alignment, and mobility apps that remind me to stay active safely. These resources have become my allies in maintaining progress and making mobility a sustainable part of my life, demonstrating that the right equipment and guidance are truly powerful for lasting relief.
Let Your Experience Shape Your Path Forward
Remember, everyone’s body responds differently. Embrace what works uniquely for you, be patient with setbacks, and stay curious about new strategies. Your journey to pain-free mobility is personal—and the most valuable insights come from listening to your own body and continuously adapting. Keep pushing with kindness and consistency, and long-term relief will follow.
What small change has made the biggest difference in your approach to managing sciatic pain? Share your story below—I’d love to hear how you’re transforming your routine for better relief.