Last night, I woke up with that familiar, dull ache shooting down my leg. It was so intense I almost thought about crawling back into bed, but then I realized something – I had fallen asleep on my side, in that same position I’d been doing every night for months. That moment was a lightbulb for me: my sleep habits, especially my side-sleeping pattern, might be fueling my ongoing sciatic pain. Have you ever experienced a similar wake-up call after a night of restless sleep, feeling that familiar nerve flare-up? If so, you’re not alone, and today, I want to show you how your nightly habits could be behind your flare-ups—and what you can do about it.
The Hidden Link Between Side-Sleeping and Sciatica Flare-Ups
Many of us don’t realize that sleeping positions are more than just comfort choices; they have a profound impact on our spine and nerve health. Specifically, side-sleeping, when done habitually and without proper support, can put undue pressure on the sciatic nerve, exacerbating pain over time. It’s like leaning on a fragile bridge every night—eventually, the stress adds up. I used to shrug off my persistent discomfort, chalking it up to
Adjust Your Sleeping Position for Lasting Relief
Start by inspecting your current side-sleeping habit. Use a firm, supportive pillow that keeps your neck aligned with your spine, preventing unnecessary strain. Experiment with placing a pillow between your knees; this simple move can realign your hips and reduce pressure on your sciatic nerve, akin to balancing a see-saw evenly on both sides. I once tried this after nights of persistent pain, and within days, I noticed a significant decrease in nerve sensitivity.
Optimize Your Mattress Selection
Think of your mattress as the foundation of a house—if it’s sagging or too soft, it can warp your spine’s natural curve. Invest in a medium-firm mattress that conforms to your body but provides enough support. This change is like switching from a soft sofa to a supportive, ergonomic chair—it instantly improves posture during sleep and prevents nerve compression. I replaced my old mattress with a memory foam variant and found my nightly discomfort diminished considerably.
Implement Bedtime Support Techniques
Prior to sleeping, perform gentle stretches targeting the lower back and hips, such as knee-to-chest or piriformis stretches. These act like warming up a car engine before a long drive, preparing your body and easing tension. For instance, I incorporated a 5-minute routine of these stretches, which helped my muscles relax and reduced nerve irritation overnight. Regularly applying these techniques keeps your spine mobile and less prone to painful flare-ups.
Maintain Awareness of Your Daytime Posture
Your sleep habits are affected by how you sit and move during the day. If you spend long hours at a desk, ensure your chair supports your lower back and your feet rest flat on the ground. Consider ergonomic adjustments, such as a standing desk or footrest, to avoid compressing your spine—a common culprit for nerve issues. Many find that improving their daytime posture directly correlates with better sleep quality and reduced sciatic symptoms.
For comprehensive guidance on maintaining spinal health, explore mobility mastery tips or delve into ergonomic practices adaptable to your routine. Remember, small, consistent changes can make a substantial difference in managing and preventing sciatic discomfort over time.

Most people believe that stretching is the universal solution to back pain and sciatic discomfort, but in my experience, this can be a dangerous oversimplification. For instance, many are tempted to assume that the more you stretch, the better your mobility will be. However, overdoing certain stretches without understanding their nuances can actually exacerbate issues. It’s essential to recognize that not all mobility exercises are appropriate for every stage of pain; some might temporarily improve flexibility but worsen underlying instability if executed improperly. I advise exploring simple, targeted mobility exercises that address specific weaknesses rather than broad, generic stretching routines, which can lead to joint hypermobility and instability if misapplied.
Are All Movement Restrictions Equal, or Are Some Masking Deeper Problems?
In-depth assessments reveal that many restrict their movement thinking they’ll prevent pain, but this often results in further stiffness and dysfunction. This misconception is rooted in the belief that limiting movement preserves health; paradoxically, it can cause the very issues we aim to avoid by promoting body awareness and functional movement patterns. For example, avoiding certain motions without understanding their purpose may lead to muscle imbalances and joint degeneration over time. An expert review published in the Journal of Orthopaedic & Sports Physical Therapy emphasizes the importance of differentiating between harmful restrictions and protective, adaptive stiffening—highlighting that tailored physical therapy can restore natural movement without risking further injury (read more on safe mobility practices). Recognizing this nuance is crucial for effective healing and long-term health—dismissing it can trap you into cycles of pain and ineffective treatments.
Finally, be cautious of common pitfalls like neglecting posture during daily activities, which silently worsens mobility issues over time. Small adjustments, such as ergonomic upgrades and conscious movement habits, can make a profound difference. For comprehensive guidance on avoiding these traps, check out this post on posture and chronic pain. Have you ever fallen into this trap? Let me know in the comments.
To keep your progress consistent and your mobility optimal, having the right tools at your disposal is essential. These aren’t just gadgets; they’re strategic assets that help you monitor, support, and enhance your recovery journey. I personally rely on a combination of ergonomic equipment, specialized mobility aids, and digital resources that empower me to stay on top of my health—not just for days, but for months and years to come.
Invest in Quality Support Devices
An adjustable lumbar support cushion is indispensable. I use the Kieba Lumbar Support Pillow, which offers customizable firmness and contours perfectly to my lower back, especially during long periods of sitting. These cushions promote good posture, reduce muscle strain, and prevent nerve compression—key factors in fighting the recurrence of sciatic or neck pain. The secret lies in consistent, proper support that mimics professional ergonomic coaching without the price tag of ongoing therapy sessions.
Utilize Wearable Biofeedback Gadgets
Devices like the Moov HR activity tracker provide real-time feedback on your posture and movement habits. This helps me identify when I’m slouching into bad postures during work or leisure. By receiving alerts and insights, I can correct my positioning immediately — a habit that over time drastically reduces flare-ups. Future trends suggest more advanced wearables will incorporate AI-driven analytics, making personalized mobility coaching more accessible than ever.
Leverage Targeted Mobility Tools
Foam rollers are a staple in my routine, but not all foam rollers are created equal. I prefer the TriggerPoint GRID Foam Roller because of its multi-density surface, which can target specific muscle knots that contribute to nerve irritation. Regular use of such tools keeps my muscles pliable, joints mobile, and nerves unpressured. For those dealing with stubborn or chronic issues, combining foam rolling with targeted stretches, as discussed here, can yield long-lasting results.
Implement Digital Guidance and Tracking
Apps like MobilityWOD or StretchIt transform your smartphone into an on-demand coach. These platforms offer personalized routines tailored to your specific pain points, ensuring you’re doing the right moves at the right times. I use them daily to reinforce proper technique and stay motivated. As technology advances, we’re moving toward AI-driven apps that analyze posture data via camera or wearables, providing instant feedback and adjustments—making long-term maintenance smarter and more precise.
Where Do I Keep Up with the Latest Tools and Techniques?
Staying informed is crucial. Regularly visiting reputable sites like this cornerstone resource ensures you’re aware of emerging devices and methodologies. I also recommend consulting with physical therapists who are increasingly integrating tech into their practice, helping you select tools optimized for your unique needs. Remember, the consistency of using these tools makes the difference—commit to integrating at least one new device or app into your routine every few months.
Want to take your mobility maintenance to the next level? Try incorporating a targeted foam rolling routine with the TriggerPoint GRID Foam Roller and track your improvements with a wearable device like the Moov HR. Consistency with these tools, combined with expert-guided exercises, can significantly reduce the risk of flare-ups and promote lasting health.

Imagine a comprehensive setup of ergonomic supports, mobility tools, and digital trackers all working in harmony — this dynamic system is shaping the future of sustainable back and nerve health for many individuals. Incorporate these tools today to ensure your progress isn’t just fleeting but enduring.
Throughout my experience managing sciatica and mobility challenges, I realized that some of my biggest breakthroughs came from embracing my mistakes rather than avoiding them. One ‘hard lesson’ was understanding that not all pain signals are straightforward; sometimes, they whisper subtle warnings that need attentive listening. I learned to pay close attention to my body’s feedback, recognizing that rushing into aggressive stretches or unsupported positions only delayed healing. These insights reshaped my approach, emphasizing patience, tailored movements, and awareness over quick fixes. Embracing this mindset transformed my recovery, showing me that setbacks are often stepping stones rather than dead ends, and being willing to learn from each misstep unlocks the path to better mobility and lasting relief.
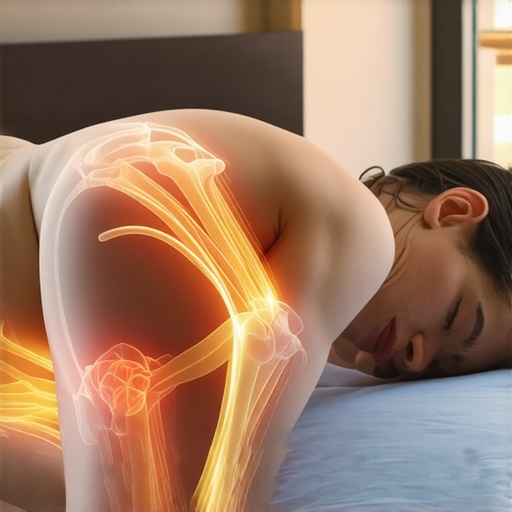



I really relate to the idea that sleep habits can significantly impact sciatic pain. I used to think my mattress was fine until I started experiencing nerve flare-ups that woke me up at night. After switching to a medium-firm mattress and consciously placing a pillow between my knees, I noticed a big difference in my comfort levels and frequency of pain. It’s interesting how small adjustments during sleep can lead to such noticeable improvements. I’ve also found that incorporating gentle pre-bed stretches helps me relax my hips and lower back, making my sleep position less likely to aggravate my sciatic nerve. Has anyone else found a particular type of pillow or mattress that works best for them? I’d love to hear more about what’s helped others prevent those nocturnal flare-ups—sometimes, I think it’s really a puzzle trying to find the right support.
Your post really resonated with me, especially the part about how sleep position and support influence sciatic pain. I’ve found that despite using a supportive pillow between my knees, I still wake up with discomfort. Recently, I started paying more attention to the firmness of my mattress, and I noticed that switching to a medium-firm one made a noticeable difference. I also added some gentle hip stretches before bed, which seem to relax my muscles and reduce nerve irritation during the night. It’s interesting how a combination of proper support and targeted stretching can really improve sleep quality and symptoms during the day. Has anyone experimented with different sleep surfaces or supports that have worked well for their sciatic pain? I wonder if incorporating more dynamic movement or sleep position changes could further decrease those nerve flare-ups. I’d love to hear what others have tried that’s been effective in managing nighttime discomfort, as it can be such a frustrating cycle to break.